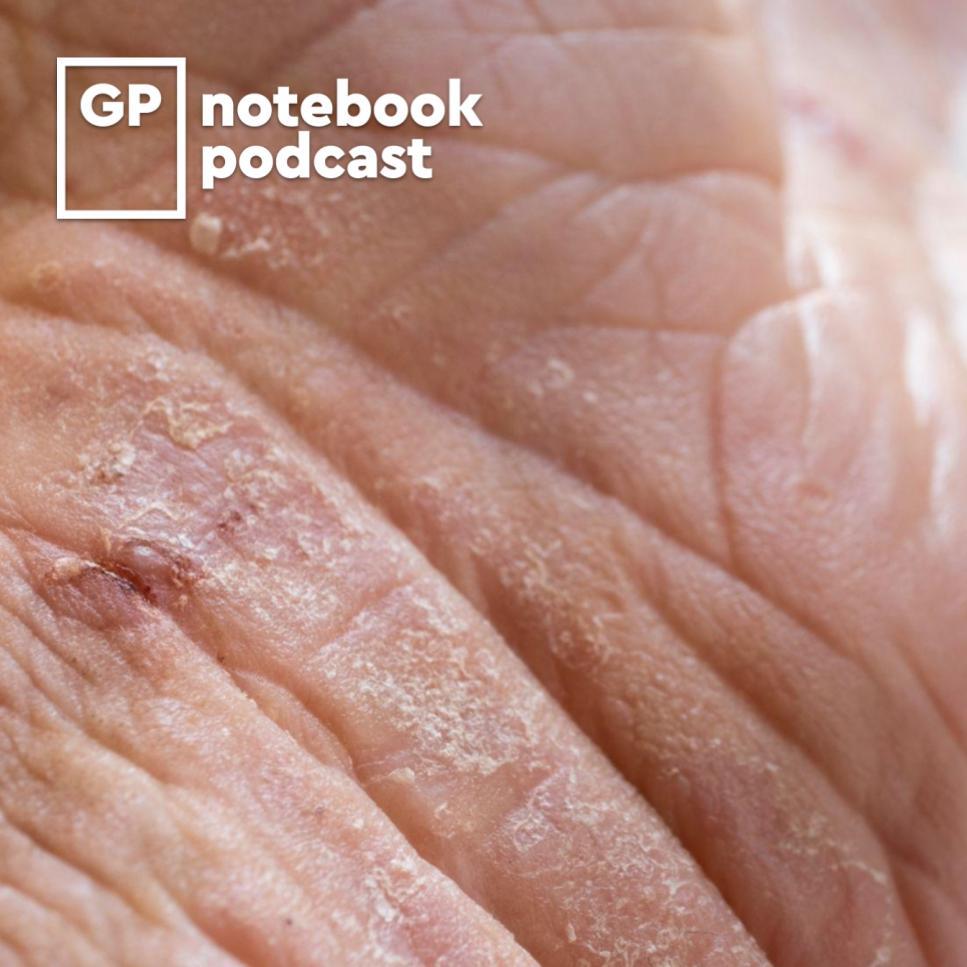
Actinic keratosis (AK) – also commonly known as solar keratosis – is a very common dermatological presentation in primary care, affecting large numbers of older people. It has the capacity to transform into a malignant lesion if untreated. In this podcast, Dr Roger Henderson looks at who is most at risk of AK, how it should be diagnosed, what treatment options are available, and when to consider referral to secondary care.
Key references and resources
- BNF, Treatment Summaries. Photodamage. Accessed 20 February 2023.
- Primary Care Dermatology Society. Actinic keratosis (syn. solar keratosis). 23 November 2022.
- Actinic keratoses (solar keratoses). 8 June 2020.
- British Association of Dermatologists. Actinic keratoses. December 2020.
Key take-home points
- Actinic keratosis (AK) is common, affecting almost one in four of the UK population aged 60 and over.
- It is an ultraviolet light-induced hyperkeratotic skin condition that has the occasional potential to become malignant, transforming to a squamous cell carcinoma (SCC).
- AK is more common in people with fair skin, blue eyes and blonde hair, and less common in skin of colour. Men are more commonly affected.
- If 10 or more AKs are present, this is associated with an up to 14% increased risk of developing an SCC within 5 years.
- The majority of AK cases are asymptomatic.
- If symptoms develop such as bleeding, ulceration, or increase in size or pain, then this can suggest transformation into an SCC.
- AK distribution is linked to skin with greatest sun exposure, such as the head, forearms, hands and neck.
- AK lesions are seldom larger than 1 cm.
- There is often a background of significantly sun-damaged skin around an AK.
- The clinical appearance is a flattish, rough surface scale that is usually white in colour.
- Diagnosis is typically clinical, with no need for biopsy. If biopsy is required, it shows partial thickness dysplasia or atypia of the keratinocytes in the epidermal basal layers.
- General treatment measures for all patients include checking all skin areas for sun damage – not just the affected area. If the diagnosis is in doubt, moisturising the area regularly can help differentiate between an AK and simple dry skin.
- Not all patients need treating (such as an isolated, low-level AK lesion).
- Patients should always be advised about the increased reddening, crusting or mild discomfort that topical treatments may cause. If not, compliance may be compromised.
- Lesion-specific treatment includes treating the lesion alone and can involve 5% fluorouracil cream, tirbanibulin, 0.5% fluorouracil/10% salicylic acid solution or single cryotherapy.
- Areas of skin that have multiple AKs associated with changes seen in sun-damaged skin are more at risk of developing SCC. Small areas can be treated with the same topical treatments as for lesion-specific treatment, plus photodynamic therapy. Larger areas can be treated with 3% diclofenac gel or 3.75% imiquimod cream.
Create an account to add page annotations
Add information to this page that would be handy to have on hand during a consultation, such as a web address or phone number. This information will always be displayed when you visit this page